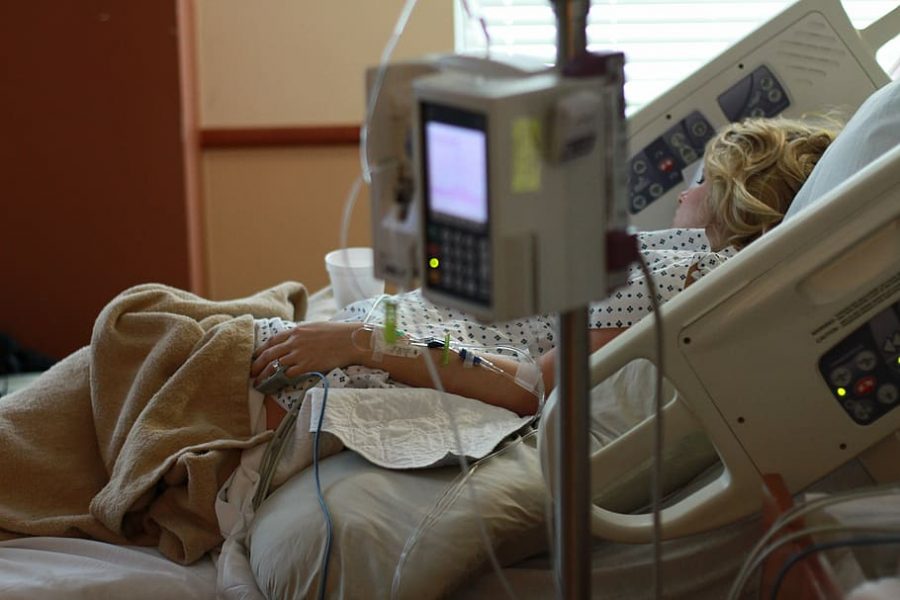
ICU Capacity in Critical Condition
Not all COVID-19 patients have access to ICU beds.
With the recent surge of Coronavirus cases in many states, hospitals are overwhelmed with a growing number of patients. Doctors and nurses are contacting numerous hospitals across the United States in hopes of transferring patients in critical condition. On September 16, Idaho’s Department of Health and Wellness announced that their hospitals are having a medical shortage, and they have practically no room left for patients. This leaves them to use alternative methods, like using parking lot capacity. Even so, this is not a long-term nor a sustainable solution. According to the Washington Post, “Idaho morgues are running out of space for bodies as covid-19 deaths mount.” This is caused by a huge spike in deaths mostly driven by the highly infectious Delta variant of COVID-19. The Delta along with other variants are responsible for the deaths in America leading to a shortage of morgues around the state.
Intensive care is a specialized treatment for people who are critically ill and require immediate medical attention. Critical care and life support are provided in an intensive care unit, also known as an ICU. They provide care for patients who deal with life-threatening conditions and injuries. Especially during the Covid pandemic, these spaces are extremely limited and cannot hold more than a certain amount of people. When there is an outbreak of cases, the ICU frontline workers must pick and choose who gets to receive care which is devastating towards those who do not receive the medical attention they need. Those who were not treated by medical professionals may, unfortunately, end up perishing.
As reported by the US Department of Health and Human Services, more than half of the ICU beds are occupied with Covid patients. Dr. Dotti Owens of Ada County, Idaho, shares that “We are working nonstop. We’re exhausted. We’re frustrated.” ICU doctors and nurses are burned out by the number of patients needing care. There simply isn’t enough room or medical professionals who can assist everyone who is in need. Because of the shortage of healthcare workers and beds ratio to every patient is so drastic, some patients are left unattended. At Cloverdale Funeral Home in Ada County, their managing partner Steve Salove mentions how their refrigeration facility has reached full capacity and cannot fit more bodies. “Funeral homes are out of storage. Our hospitals are out of storage.” According to Salove, part of the issue is how many of the victims’ families have also contracted Covid-19. The events occurring in Idaho are unfortunate, but not unexpected. A CDC report released September 10 stated that unvaccinated people in the U.S. are 10 times more likely to be hospitalized with COVID-19 and 11 times more likely to die compared to people who have gotten the vaccine. This data supports why death tolls from COVID-19 are highest in Idaho.
However, this phenomenon is not just happening in Idaho. States including Georgia, Alabama, Florida, Mississippi, and Texas all currently have less than 10% of ICU capacity available for patients. Most that are infected caught the Delta variant, a mutation much stronger than Coronavirus. So why these states? Dr. William Schaffaner explains that “The discrepancies in case rates are the direct reflection of discrepancies in vaccination rates. The lower the vaccination rate, the higher the case rate and the hospitalization rate,” Additionally, even in remote states such as Alaska, hospitals are seeking additional medical staff to assist with the overwhelming amount of Covid-19 cases. Officials say that “this endeavor will likely cost the state about $1 million per day, which will be reimbursed by the federal government.”
As reported by the New York Times, Coronavirus is responsible for over 680,000 deaths in the United States. To reduce the number of people getting infected and potentially ending up in one of these ICU care units, the Department of Health and Human Services recommends everyone eligible to get both doses of the Covid vaccine. The Centers for Disease Control and Prevention also suggests that everyone, regardless of vaccination status, should be wearing a mask to slow the spread of Covid. By getting vaccinated and wearing masks, communities would surpass over COVID-19, and ICU capacity rates would eventually get back to normal.